Tagged: medical education
Are the Hallmarks of Cancer a Good Framework for Teaching Oncology?
One of the challenges in teaching medicine and in particular sub-specialty medicine is the sheer volume of information to be digested. The commonest refrain I hear about studying the discipline of interest, in particular from new trainees in medical oncology, is ‘I don’t know where to start’.
There are many potential approaches.
There is the traditional basic science to clinical science approach. For example starting with the relevant biochemistry, anatomy, etc and building up towards practice.
There is the problem-based learning approach which is good for clinical scenarios but perhaps doesn’t encourage an understanding of depth.
Another approach applies templates to diseases. For example if we consider breast cancer one can think about the epidemiology, screening, prevention, adjuvant treatment and treatment of recurrent disease. The same template could be applied to each cancer type. There are common themes and also variations and differences between each cancer….but the basic themes are the same.
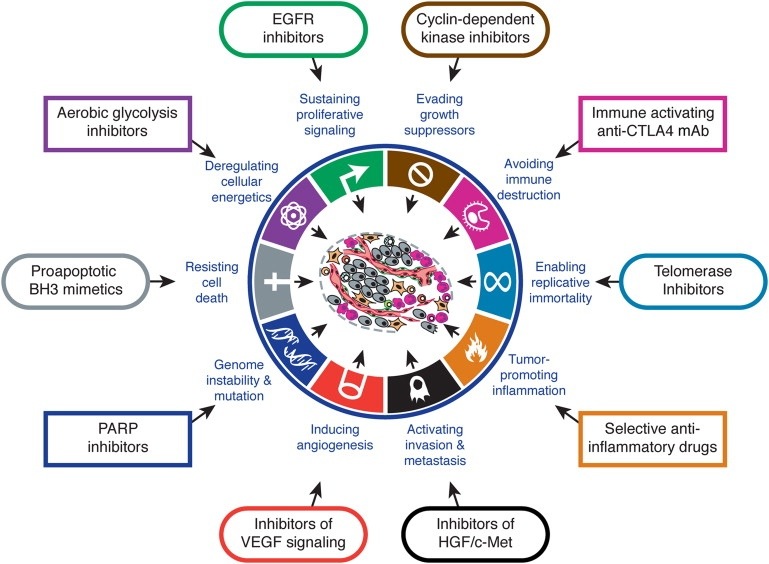
Arguably the latest approach is that of looking at the Hallmarks of Cancer as proposed by Hanahan and Weinberg in Cell (2000). The authors propose that there are key characteristics that cancers acquire that distinguish themselves from non-cancers. Although there are some criticisms that some of the hallmarks also apply to benign tumours, broadly speaking the concept provides a useful way for thinking about how cancers behave.
I think Hallmarks of Cancer is a useful framework for teaching oncology. What makes it useful if that you can think about high level concepts such as sustained angiogenesis or evasion of immunoregulation or self-sufficiency in growth signals or any of the hallmarks as having potential for application across the spectrum of oncologic interest: the hallmarks inform aetiology, diagnosis, prognostication, and potential treatment strategies. It provides a framework that facilitates both understanding complexity and engaging reductionism. It is the view from the plane that lets us know the concepts but enables closer examination.
Trainees need to familiarise themselves with The Hallmarks of Cancer and apply it to their studies.
Things they didn’t teach in medical school: Part 31 Advocacy
One of the things they didn’t teach in medical school is advocacy. There are different meanings for advocacy – in this case I refer to the broader meaning of advocating for patients and communities to achieve an end to their benefit. An example might be supporting the funding of a new drug or campaigning for increased resources for a hospital.
Simplistically advocacy can just be about being vocal but there can be problems with this approach.
To be an advocate it is important to be able to see all points of view so as being able to bring a cogent argument to the table. Often times advocates are dealing with political situations and positions and invariably these become polarised – it is important to diffuse this polarisation to get the party with whom one is lobbying to also be able to see the arguments in favour of your position. Advocates need to be prepared to compromise to achieve small but important wins rather than overnight revolution.
Advocates need to be careful about their motivations for lobbying. For example it is not uncommon for drug companies to ask doctors to provide support for a new treatment. If this happens there needs to be transparency about the reasons for lobbying and full disclosure of any conflicts of interest.
Similarly advocates need to be careful that their lobbying is not seen as some form of whistle-blowing – this is because some employment contracts prohibit this activity. In this case being part of a community of advocates is important. There is strength in numbers.
There are many tools for advocacy – the main one is conversation and the new medium for conversation is social media. Mastery of social media and branding the advocacy message is a new skill for the medical graduate advocate.
The Curator Unplugged – Training Future Doctors in the Era of Electronic Decision Support
One of the key problems facing educators in medicine today is how to train future doctors in medical decision making in an emerging era of electronic decisions support in EHR (electronic health record).