Philip Glass Symphony No.9
What they didn’t teach in medical school Part 1: Behaviour Change
This is the start of an occasional series about stuff they didn’t teach me in medical school – and I suspect they still don’t teach this stuff. Where it was taught I suspect it was pretty poorly. These musings have come about because most of what I do now, that doesn’t fall into the categories of diagnosing or treating, wasn’t taught in medical school or as part of my specialist training. Some of these things include how to be an administrator, how to run a meeting, how to run a business, how to teach trainees and a whole bunch of stuff around fine-tuning the practice of medicine. I won’t necessarily have the answers about what to do to address these problems but recognition is the first step.
To kick it off with I’m nominating how to change patient behaviour.
Most of what I do on a day to day basis as an oncologist is prescribing medications to treat cancers. But there are a whole lot of behaviours that might also need to be changed or created to help my patients get through their illness. In the same way primary care practitioners need to be able to help their patients change behaviours in order to achieve preventative medicine goals.
Examples of behaviours and problems that might need to be addressed through behaviour change include tobacco, alcohol and substance abuse, obesity and poor fitness, poor adherence to medications or aberrant mechanisms for coping with illness.
I recall being taught how to detect these problems but not a great deal about how to address them. I suspect most busy doctors see their patients and go through the motions of discussing smoking cessation or some other behaviour change but either give up in despair or through lack of time or perhaps take the easy option and write a script for a patch or some other aid (which might help but should be part of a package deal not a one stop solution).
So every doctor dealing with these problems ought to read up or take a class on behaviour change. It’s all the rage in popular non-fiction right now with books on behavioural economics (Nudge by Thaler & Sunstein, Thinking Fast and Slow by Kahneman) and habit change (The Power of Habit by Duhigg) being in the best-seller lists.
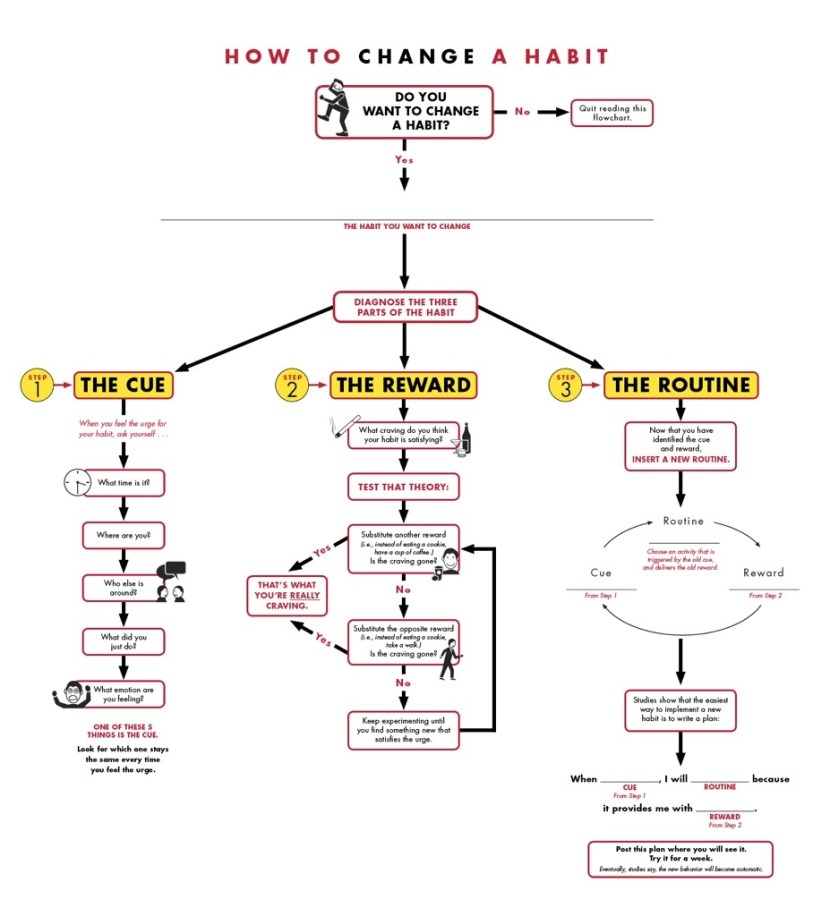
If you’re a doctor reading this then one way to learn about it is to try and change one of your own habits. Here a some clues how Charles Duhigg Habit Change Resources
Zoomusicology – is it for the birds?
Listening to Jonathan Harvey Bird Concerto with Piano Song played by Hideki Nagano with the London Sinfonietta conducted by David Atherton. For more on this work see Bird Concerto
You might also like The Piccolo and the Pocket Grouse
Edgard Varese Ameriques (1927)
Michael Tilson Thomas conducting San Francisco Symphony in Ameriques by Edgard Varese.
For more info see Ameriques
A New Year of Music
After a relative year off having completed the 365 String Quartets in 2011 I’m kicking off the musical journey again with an emphasis on modernism, 20th Century & contemporary classical orchestral music. To be liberal about the 20th Century I’ll listen from the period of Brahms & Mahler to the present.
Kicking off the year is Detailed Instructions (for Orchestra) 2010 by Nico Muhly, played by the New York Philharmonic under the direction of Alan Gilbert.
The Curator Unplugged – Training Future Doctors in the Era of Electronic Decision Support
One of the key problems facing educators in medicine today is how to train future doctors in medical decision making in an emerging era of electronic decisions support in EHR (electronic health record).
Training prescribers how to prescribe mHealth apps
Sometime soon your doctor is going to prescribe you a mHealth app for your smartphone. There’s a 1 in 3 chance you already have one on your phone – for tracking calories, weight, exercise, your smoking, your blood sugar or our mood. How will you or your doctor know which is the right app?
Will your doctor be prepared to override you and your smartphone?
- patient use of the internet to obtain health information and make healthcare decisions
- the slow but inexorable rise of electronic health records (EHR)
- digital modes of communication between patients and healthcare providers
- the development of knowledge repositories for electronic decision support
- the use of behavioural economic techniques, social media engagement and analytics, gamification and other methods to modify health behaviour. This change is epitomised by the life-logging, quantified health movement
- the development of sophisticated diagnostic devices for personal use
Re-booting the blog
Have been quiet on the blogging front since the Year of the String Quartet 365SQ. Have migrated across from Posterous and plan regular commentaries on health care with an emphasis on personal and personalised medicine, healthcare practice change, oncology, eHealth, and medical education, and the occasional excursion back to music – so watch this space.